first issue
january 12, 2022
Ever wonder if the opioid epidemic affected dermatologists and how they responded?
JAMA Dermatology
Turns out dermatologists prescribe more than just retinoids! Given public health concerns regarding the opioid epidemic, physicians have been encouraged to engage in safer opioid practices. In dermatology, dermatologic surgeons prescribe the most opioids, but their changes in prescribing in response to the epidemic had not yet been evaluated to see if they could effectively balance potential negative consequences with adequate pain relief. This cross-sectional study examined a national database of insurance claims from Mohs surgery from 2009 to 2020 (n = 358,012). The proportion of patients who underwent Mohs with opioid claims rose from 34.6% in 2009 to a peak of 39.6% in 2011, then decreased annually to a rate of 11.7% in 2020. Odds of an opioid claim in patients who underwent MMS decreased 61% per calendar year (odds ratio [OR],0.39 per calendar year; 95% CI, 0.37-0.41; P < .001). By 2020, hydrocodone was obtained less (2009: 47.5%; 2011: 67.1%; 2020: 45.4%; 21.7% absolute decrease from 2011 to 2020) and tramadol was obtained more (2009: 1.6%; 2020: 27.9%; 26.3% absolute increase from 2009 to 2020). This data shows a general decrease in both the quantity of prescriptions and prescription claims through insurance, as well as a transition to lower strength opioids if they were being prescribed. Dermatologists should continue this trend in safer opioid prescribing, both in lesser frequency and safer opioids, following Mohs surgery.
Could surgical delays contribute to higher rates of morbidity and mortality for non-melanoma skin cancers?
Journal of American Academy of Dermatology
Delays may mean more than still waiting for that holiday gift to arrive due to COVID-19 supply chain disasters. Unfortunately, surgical delays are common for Mohs surgery, the gold standard for excision of facial (head/neck) and/or aggressive basal cell carcinomas (BCC) and squamous cell carcinomas (SCCs). Evidence is lacking about the impact of these surgical delays on tumor growth. In a retrospective analysis of 299 SCCs and 802 BCCs treated with Mohs surgery, researchers sought to determine whether independent predictors of tumor growth (ΔMD) trended with surgical delay. Tumor growth was measured as the change in major diameter (ΔMD) from size at biopsy to postoperative Mohs surgery defect. Median surgical delay was 48 days (range 0-331 days). Poorly- or moderately- differentiated SCCs were the only significant predictors of ΔMD associated with surgical delay, demonstrating growth rates of 0.28 cm (p=0.005) and 0.24 cm (p=0.016) per month, respectively. Other independent predictors of tumor growth for SCC (prior treatment) and BCC (age, male gender, aggressive histology, location, and prior treatment) did not vary with surgical delay. Overall, these results suggest that surgical delays of less than 11 months may have clinical significance for moderately- and poorly- differentiated SCCs. While further studies are needed to assess clinical significance of this tumor growth, timely Mohs surgery of these higher risk lesions may reduce their surgical morbidity, recurrence and metastasis.
Boosted Blasts with Bleomycin Electrosclerotherapy
Dermatologic Surgery
Who knew that when Benjamin Franklin flew a kite in a storm to harness electricity, that we would be using it today to power electric cars, charge our smartphones, and to treat congenital vascular malformations (CVMs) in dermatologic procedures? CVMs are venous and/or lymphatic malformations that cause swelling, pain, speech impediment, bleeding, and cosmetic problems. Sclerotherapy, in which sclerosing agents are injected and cause shrinkage or collapse of the CVM, is the first-line treatment. Electroportation is a technique which passes electric pulses through the diseased area and creates pores in underlying cell membranes to allow more agent to enter the cell. The combination of sclerotherapy and electroportation is called electrosclerotherapy. This prospective observation case series investigated the use of bleomycin electrosclerotherapy in 30 participants whose CVMs did not respond to sclerotherapy alone. 17 (53%) patients had a complete resolution of their CVM and 7 (23%) had significant improvement (60-90% total area). Overall patient treatment satisfaction was 6.2 on a 7-point scale. Further studies should include a more diverse sample of CVM subtypes, and future data should be evaluated more quantitatively than the subjective methods used. Despite limitations, this study highlights the utility of electrosclerotherapy when using bleomycin to treat CVMs resistant to sclerotherapy.
JAMA Dermatology
Turns out dermatologists prescribe more than just retinoids! Given public health concerns regarding the opioid epidemic, physicians have been encouraged to engage in safer opioid practices. In dermatology, dermatologic surgeons prescribe the most opioids, but their changes in prescribing in response to the epidemic had not yet been evaluated to see if they could effectively balance potential negative consequences with adequate pain relief. This cross-sectional study examined a national database of insurance claims from Mohs surgery from 2009 to 2020 (n = 358,012). The proportion of patients who underwent Mohs with opioid claims rose from 34.6% in 2009 to a peak of 39.6% in 2011, then decreased annually to a rate of 11.7% in 2020. Odds of an opioid claim in patients who underwent MMS decreased 61% per calendar year (odds ratio [OR],0.39 per calendar year; 95% CI, 0.37-0.41; P < .001). By 2020, hydrocodone was obtained less (2009: 47.5%; 2011: 67.1%; 2020: 45.4%; 21.7% absolute decrease from 2011 to 2020) and tramadol was obtained more (2009: 1.6%; 2020: 27.9%; 26.3% absolute increase from 2009 to 2020). This data shows a general decrease in both the quantity of prescriptions and prescription claims through insurance, as well as a transition to lower strength opioids if they were being prescribed. Dermatologists should continue this trend in safer opioid prescribing, both in lesser frequency and safer opioids, following Mohs surgery.
Could surgical delays contribute to higher rates of morbidity and mortality for non-melanoma skin cancers?
Journal of American Academy of Dermatology
Delays may mean more than still waiting for that holiday gift to arrive due to COVID-19 supply chain disasters. Unfortunately, surgical delays are common for Mohs surgery, the gold standard for excision of facial (head/neck) and/or aggressive basal cell carcinomas (BCC) and squamous cell carcinomas (SCCs). Evidence is lacking about the impact of these surgical delays on tumor growth. In a retrospective analysis of 299 SCCs and 802 BCCs treated with Mohs surgery, researchers sought to determine whether independent predictors of tumor growth (ΔMD) trended with surgical delay. Tumor growth was measured as the change in major diameter (ΔMD) from size at biopsy to postoperative Mohs surgery defect. Median surgical delay was 48 days (range 0-331 days). Poorly- or moderately- differentiated SCCs were the only significant predictors of ΔMD associated with surgical delay, demonstrating growth rates of 0.28 cm (p=0.005) and 0.24 cm (p=0.016) per month, respectively. Other independent predictors of tumor growth for SCC (prior treatment) and BCC (age, male gender, aggressive histology, location, and prior treatment) did not vary with surgical delay. Overall, these results suggest that surgical delays of less than 11 months may have clinical significance for moderately- and poorly- differentiated SCCs. While further studies are needed to assess clinical significance of this tumor growth, timely Mohs surgery of these higher risk lesions may reduce their surgical morbidity, recurrence and metastasis.
Boosted Blasts with Bleomycin Electrosclerotherapy
Dermatologic Surgery
Who knew that when Benjamin Franklin flew a kite in a storm to harness electricity, that we would be using it today to power electric cars, charge our smartphones, and to treat congenital vascular malformations (CVMs) in dermatologic procedures? CVMs are venous and/or lymphatic malformations that cause swelling, pain, speech impediment, bleeding, and cosmetic problems. Sclerotherapy, in which sclerosing agents are injected and cause shrinkage or collapse of the CVM, is the first-line treatment. Electroportation is a technique which passes electric pulses through the diseased area and creates pores in underlying cell membranes to allow more agent to enter the cell. The combination of sclerotherapy and electroportation is called electrosclerotherapy. This prospective observation case series investigated the use of bleomycin electrosclerotherapy in 30 participants whose CVMs did not respond to sclerotherapy alone. 17 (53%) patients had a complete resolution of their CVM and 7 (23%) had significant improvement (60-90% total area). Overall patient treatment satisfaction was 6.2 on a 7-point scale. Further studies should include a more diverse sample of CVM subtypes, and future data should be evaluated more quantitatively than the subjective methods used. Despite limitations, this study highlights the utility of electrosclerotherapy when using bleomycin to treat CVMs resistant to sclerotherapy.
question of the week
NEJM challenge question: red dusky finger
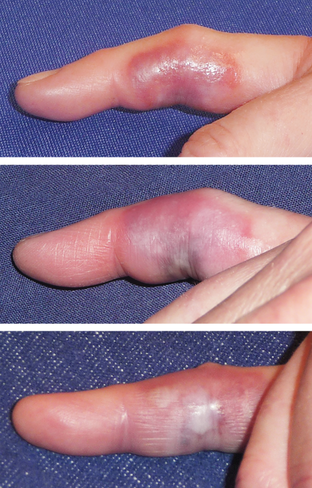
A 53-year-old woman presented with pain, swelling, and discoloration of her right fifth finger. Physical examination showed a demarcated, brightly erythematous plaque with a dusky center. What is the most likely diagnosis?
1. Dactylitis
2. Erythema multiforme
3. Herpetic whitlow
4. Spider bite
5. Sporotrichosis
1. Dactylitis
2. Erythema multiforme
3. Herpetic whitlow
4. Spider bite
5. Sporotrichosis
Answer:
Yellow Sac Spider Bite
NEJM Images in Clinic Medicine
The patient had been bitten by a spider 36 hours earlier, identified to be a yellow sac spider. The lesion progressed to dusky purpura with porcelain-white ischemic skin, and two weeks later, the patient’s finger had healed completely.
Spiders of the genus cheiracanthium, also known as yellow sac spiders, are common in North America. They are identified by their pale yellow color and dark brown fangs and leg tips. The spiders typically bite persons who are sleeping or dressing, with the bite causing local pain, redness, and swelling, usually without progression to necrosis, as occurred in this case. Two weeks after the bite, the patient’s finger had healed completely.
Other answer explanation:
Dactylitis- refers to global swelling of either a finger or toe giving it a sausage-shape presentation. Blistering distal dactylitis is typically a strep pyogenes infection that occurs as a result of nose picking or local trauma. It presents initially as darkening of the skin of a distal digit (finger>toe) and progresses to a purulent vesicle or bullae on an erythematous background within 1 week.
Erythema multiforme- presents with numerous symmetric fixed, red macules which progress into targetoid lesions. The most common locations include face and distal extremities and 90% are due to infections (e.g. HSV-1>HSV-2>mycoplasma).
Herpetic whitlow- Herpes infection of the digits (HSV-1 in children v HSV-2 in adults) which presents with vesiculation, pain and swelling.
Sporotrichosis- presents with multiple ascending ulcerated nodules or subcutaneous abscesses, most frequently in gardeners, agricultural workers, and veterinarians.
Yellow Sac Spider Bite
NEJM Images in Clinic Medicine
The patient had been bitten by a spider 36 hours earlier, identified to be a yellow sac spider. The lesion progressed to dusky purpura with porcelain-white ischemic skin, and two weeks later, the patient’s finger had healed completely.
Spiders of the genus cheiracanthium, also known as yellow sac spiders, are common in North America. They are identified by their pale yellow color and dark brown fangs and leg tips. The spiders typically bite persons who are sleeping or dressing, with the bite causing local pain, redness, and swelling, usually without progression to necrosis, as occurred in this case. Two weeks after the bite, the patient’s finger had healed completely.
Other answer explanation:
Dactylitis- refers to global swelling of either a finger or toe giving it a sausage-shape presentation. Blistering distal dactylitis is typically a strep pyogenes infection that occurs as a result of nose picking or local trauma. It presents initially as darkening of the skin of a distal digit (finger>toe) and progresses to a purulent vesicle or bullae on an erythematous background within 1 week.
Erythema multiforme- presents with numerous symmetric fixed, red macules which progress into targetoid lesions. The most common locations include face and distal extremities and 90% are due to infections (e.g. HSV-1>HSV-2>mycoplasma).
Herpetic whitlow- Herpes infection of the digits (HSV-1 in children v HSV-2 in adults) which presents with vesiculation, pain and swelling.
Sporotrichosis- presents with multiple ascending ulcerated nodules or subcutaneous abscesses, most frequently in gardeners, agricultural workers, and veterinarians.